Mumbai : In a rare emergency, doctors at Narayana Health SRCC Children’s Hospital, Mumbai successfully treated an eight-year-old boy with a spontaneous heart perforation using a minimally invasive transcatheter device, avoiding the need for high-risk open-heart surgery. The procedure was led by Dr Supratim Sen, Senior Consultant and Clinical Lead – Paediatric Cardiology.
The young patient had only recently gone through a bone marrow transplant and was still in recovery when he developed pericardial effusion—fluid accumulation around the heart. Just a few days earlier, a drainage sheath had been inserted by another operator to help remove this excess fluid from the pericardium, the protective sac surrounding the heart. While this is a standard and often necessary step to ease pressure on the heart, things took an unexpected turn when blood, instead of clear pericardial fluid, started draining from the sheath—raising immediate concern.
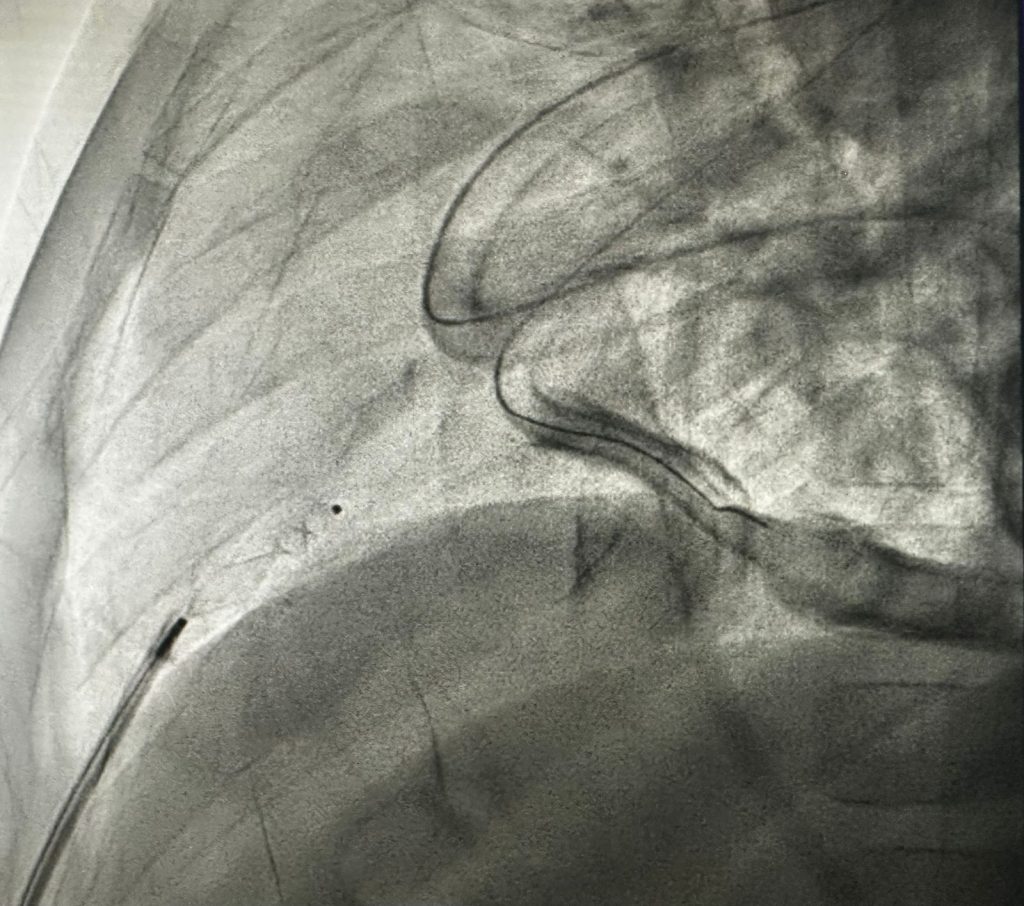
An echocardiogram showed a significant reaccumulation of fluid around the heart. Given the urgency, the child was quickly moved to the cardiac catheterisation laboratory to diagnose the exact cause of the blood in the pericardial drain. There, a combination of pressure checks and angiograms on X-ray confirmed Dr Sen’s clinical suspicion. The tip of the drainage sheath had spontaneously punctured the right ventricle, one of the heart’s main pumping chambers. In simple terms, it had created a life-threatening situation very similar to a stab wound in the heart, with a real and immediate risk of uncontrolled internal bleeding.
In most such cases, the next step would be emergency open-heart surgery—opening the chest to directly locate and repair the perforation. Preparations for this were already underway. But in that critical window, the team paused to consider another possibility. Since devices are routinely used to close holes within the heart, an idea emerged—could the same approach be used here to seal the perforation from within, without putting the child through major surgery?
Acting swiftly, the team proceeded in the cath-lab itself. Using echocardiogram and X-ray guidance, a closure device was carefully selected and delivered through the same sheath. The precision required was immense. Once the sheath was withdrawn, there would be no second chance if the device did not seal the hole completely. Despite the high stakes, the deployment went smoothly, achieving a perfect seal of the right ventricular wall. The child recovered quickly after the procedure. The success was possible by a coordinated team effort involving the cardiologist, cardiac anaesthetists, cath-lab technicians, and a cardiac sonographer, all working together in a high-pressure situation.
Explaining the case, Dr Supratim Sen said, “When we realised that the sheath had punctured the right ventricle, it posed a life-threatening emergency similar to a stab injury to the heart. Simply removing it would have caused uncontrolled bleeding. While surgery is the standard approach in such cases, we considered a novel application of an occluder device—commonly used to close holes within the heart—deployed through the same sheath to seal the perforation. The challenge was that we had only one opportunity to position it perfectly. Thankfully, the procedure went exactly as planned, allowing us to avoid open surgery and ensure a safe recovery for the child.”
This case highlights how, even in the most critical moments, the right mix of experience, quick thinking, and advanced techniques can make all the difference. It reinforces the value of minimally invasive approaches and timely decision-making in managing rare, life-threatening complications in children.